Lymphoedema is a form of chronic swelling that can often go undiagnosed. It is a result of damage to the lymphatic system and affects both men and women. Data on this condition is not being collected. It is hard to know how many people in New Zealand have this chronic condition.
There is no cure or medication for lymphoedema. It is a life-long condition. To alleviate pain and stress, good management of the condition is required.
Lymphatic System
When your lymphatic system is working well, it behaves like an overflow. This overflow returns excess fluid to the blood system for removal from the body.
The body uses protein as building blocks. When the lymphatic system is damaged, it can become overwhelmed and congested with protein-rich fluid. This fluid builds up in the tissue under the skin.
As a result of this protein-rich fluid build-up:
- the skin may become stretched and weak
- the tissues may harden, and
- one or more limbs (feet, ankles, or legs) may swell.
Swelling of the abdomen, or other parts of the body is also possible.
Diet & Exercise
For sufferers of lymphoedema, weight loss efforts may result on some loss of weight.
Effect of Lymphoedema on Quality of Life
Lymphoedema can be managed. If left untreated, it can cause serious problems that negatively impact quality of life. With lymphoedema, moving around may not be easy. As a result, it may not be possible to go to work, or look after yourself.
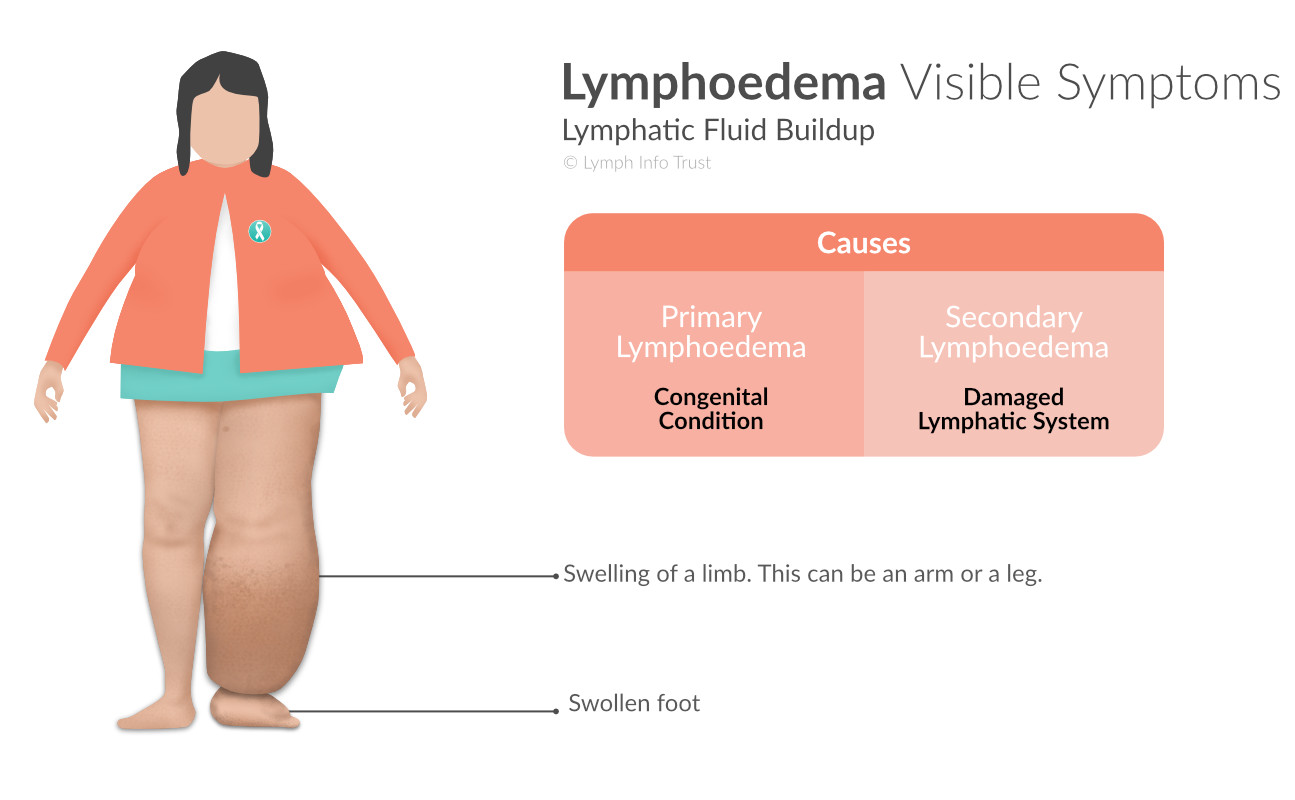
Lymphoedema Symptoms
Family members who have lymphoedema may not be an indication that predisposes someone to this disease.
The symptoms of lymphoedema include:
- swelling of a leg or arm
Note: The attached foot or hand may also swell.
Note: Lymphoedema is not limited to limbs. It can develop in other parts of the body. - splitting and hardening of the skin
- wart-like growths
- inflammation of affected areas
- pitting (smooth crater-like depressions in the skin) during the early stages of lymphoedema.
- a sensation of tightness, and
Note: Tissue tenderness is not common. The affected tissue does not bruise easily. - pain, heaviness and discomfort.
Risk of Infection
There is a high risk of infection (cellulitis) in the affected areas.
The affected skin can develop other features, such as papillomatosis of the skin.
Stages of Lymphodema
Counting Stage 0, there are four stages in the development of Lymphoedema. The stages are:
- Stage 0 – Subclinical Stage
- Stage 1 – Reversible Stage
- Stage 2 – Spontaneously Irreversible Stage
- Stage 3 – Lymphostatic Elephantiasis
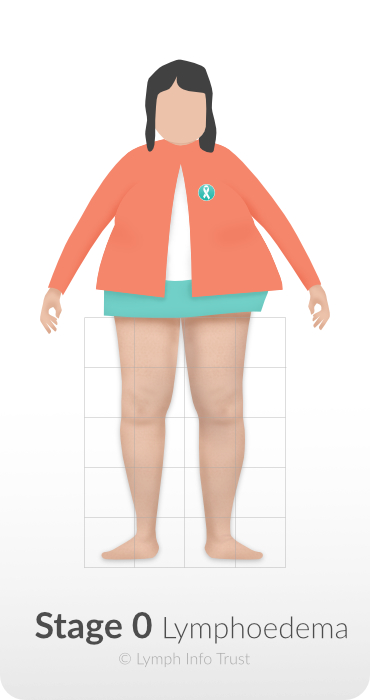
Stage 0 – Subclinical Stage
During Stage 0, damage to the lymphatic system occurs. There will be no sign of swelling or oedema at this stage.
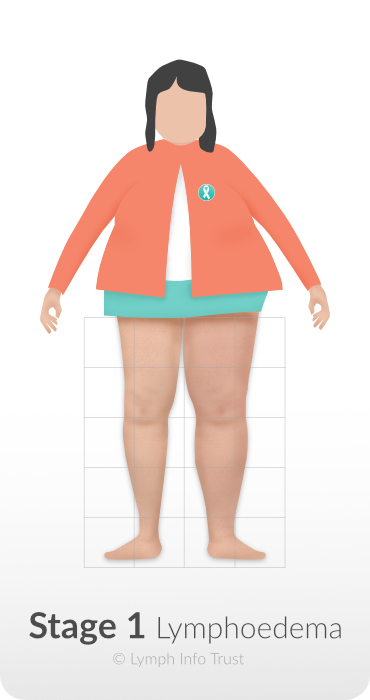
Stage 1 – Reversible Stage
Treatment is most effective if started at Stage 1 while the tissues are soft and swollen with fluid.
During this stage, the swelling can be more pronounced during the day.
Note: Swelling may reduce while sleeping. Raising the arm or leg may also bring the swelling down.
Pressing on the swelled tissue for 30 to 90 seconds leaves a dent.
Note: This response is called 'pitting'. It occurs when the fluid temporarily migrates out of the tissue when pressed.
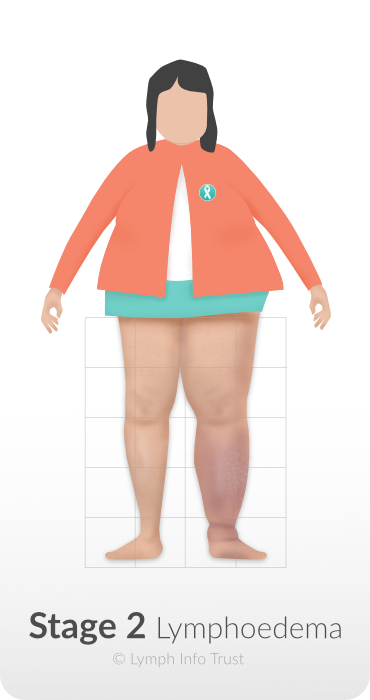
Stage 2 – Spontaneously Irreversible Stage
If the affected arm or leg remains swollen when raised, this means Stage 2 has begun.
Pressing the affected area does not leave a dent/pit.
The skin may feel harder (fibrosis) and thicker owing to a build-up of protein in the fluid.
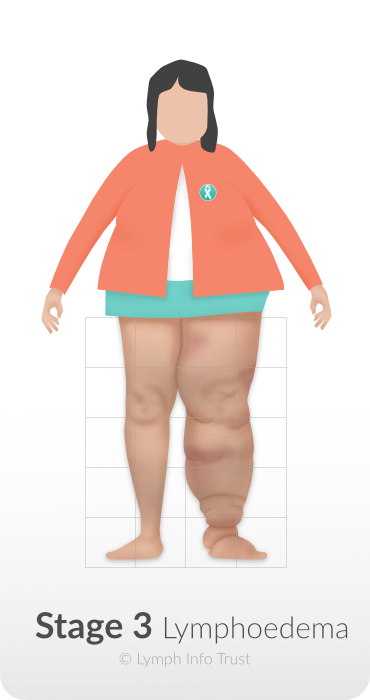
Stage 3 – Lymphostatic Elephantiasis
During Stage 3:
- the swelling will worsen.
- fibrosis or hardened skin will be more pronounced
- dramatic skin changes can occur, and
There can be a change in colour and how it feels. There may be skin growths. - there is a high risk of infection (cellulitis).
As a result of the above changes, mobility is reduced and this will contribute to lower levels of healing.
Primary Lymphoedema
Some people are born with lymphoedema (primary lymphoedema). Others may get it from another cause (secondary lymphoedema or SLO). Primary lymphoedema is the congenital form of the disorder. This means that the person was born with a lymphatic system that is not working correctly.
Swelling is more common in the lower body than the upper body.
Typical Causes
Typical causes include:
- not enough lymph vessels (Hypoplasia)
- too many lymph vessels (Hyperplasia)
Note: These vessels become rigid and the valves can’t function - missing lymphatic vessels and/or nodes (Aplasia)
- lymph vessels that are too wide (Lymphangiectasia)
Triggers
Some people show signs from birth or in childhood. Many won't show symptoms until they are in puberty or adulthood. The onset is usually triggered by an event, such as:
- reduced exercise
- puberty
- inflammation
- weight gain
- injury
- surgery
- physical stress, or
- mental stress.
Role of Genetic History
96% of primary lymphoedema cases are called spontaneous. 'Spontaneous' means there is no genetic history, which in turn means that no one else in the family has had it.
In about 4% of cases, someone else in the family will have it including:
- Nonne-Milroys
This presents at birth. - Meige’s Disease
This presents in childhood or around puberty.
Primary Lymphoedema can also be present with other conditions, including:
- Kippel-Trenaunay Syndrome
- Noonan Syndrome
- Ulrich Turner Syndrome
- Gorham Stout Syndrome
Secondary Lymphoedema
Secondary lymphoedema is the most common form of lymphoedema in NZ. It happens when the lymphatic system is damaged. The following events can damage the lymphatic system:
- injury
- surgery
Note: Cancer patients who have had their lymph nodes removed, may develop lymphoedema. - radiation therapy
- infection
- malignant lymphoedema
Example: Where the lymph flow is blocked by a tumour. - a Filariasis infection
Note: Infections happen in tropical countries where a parasitic worm is delivered to the body by mosquitoes.
Diagnosis
A physical examination, and a review of a patient's medical history, form the diagnosis.
Examination
During an examination, a health professional will look for:
- swelling on one or both sides of the body
In most cases, lymphoedema only effects one side of the body. It is possible for both legs to be affected. - pitting
The test for pitting involves pressing the tissue for 30 to 90 seconds. If it leaves an indentation (pit in the skin), this indicates the presence of fluid and that the lymphoedema has reached Stage 1. - the presence of fibrosis
When the skin thickens, this is fibrosis. The Stemmer's Sign test is a check for fibrosis. The test involves picking up the skin in a (gentle) pinch. If the skin can be picked up, then it is negative result for fibrosis. If the skin can't be picked up, this is a positive result for fibrosis. It is also an indication that the patient may have reached Stage 3. - skin changes
As lymphoedema progresses, the skin may develop growths, change texture, split, or stretch. - colour changes
Skin may change colour and darken. This can indicate chronic venous insufficiency (CVI). This is a condition whereby the venous system doesn't work as well as it should. This can cause blood and lymph to pool in the lower legs. - scarring, and
Scar tissue acts as a roadblock to lymphatic vessels. It can cause backfilling of the lymphatic system. - areas of radiation
Radiation therapy can damage lymphatic vessels and lymph nodes. This therapy can block the system's ability to drain fluid from the affected part of the body.
Medical History
Alongside a physical examination, a health professional will ask the following questions:
- How long has the swelling been there?
- How has the swelling increased or changed over time?
- Does anyone else in the family have similar symptoms?
- Have you had any triggers that might have caused oedema?
Triggers can include:- injury
- surgery
- radiation therapy
- hormonal changes, or
- excessive stress
- What side effects or complications are you having from oedema?
- What treatment are you having at the moment?
- Have you had any other treatment?
- What medications are you taking and what are these for?
If you are having or have had other treatments, you may be asked:
- what treatment worked and how did it benefit you?
- what treatment didn't work?
Tools Used for Diagnosis
Some tools can be used to confirm a diagnosis and to assist with treatment planning. The following diagnostic tools are not widely available in New Zealand:
- Lymphscintigraphy
- Indocyanine Green Scan (ICG)
- Bioimpedance/L-Dex scanners
These are available in some private clinics. - Ultrasound
Ultrasound:- is used to look at larger lymphatic organs
- is not suitable for looking at small sized lymphatic vessels
- may be used for tumour follow-up, and
- may be used for documenting skin fibroses.
- MRI or CT Scans
MRI and CT scans can be used for diagnosis, however, they are expensive.













