Phlebolymphedema is the most common form of lymphedema in the western world. It can affect up to:
- 7% of people over the age of 50, and
- 20% of people over the age of 70.
Vein & Lymph Failure
Phlebolymphoedema arises from the failure of the:
- venous circulation system, and
This is an interconnected system of veins and sinuses. - lymphatic circulation system.
This is the system that circulates a clear fluid called 'lymph' back into your bloodstream.
Effect on Quality of Life
Phlebolymphoedema can cause:
- a loss of mobility and independence, and
- an increased dependence on healthcare services.
Visible Symptoms
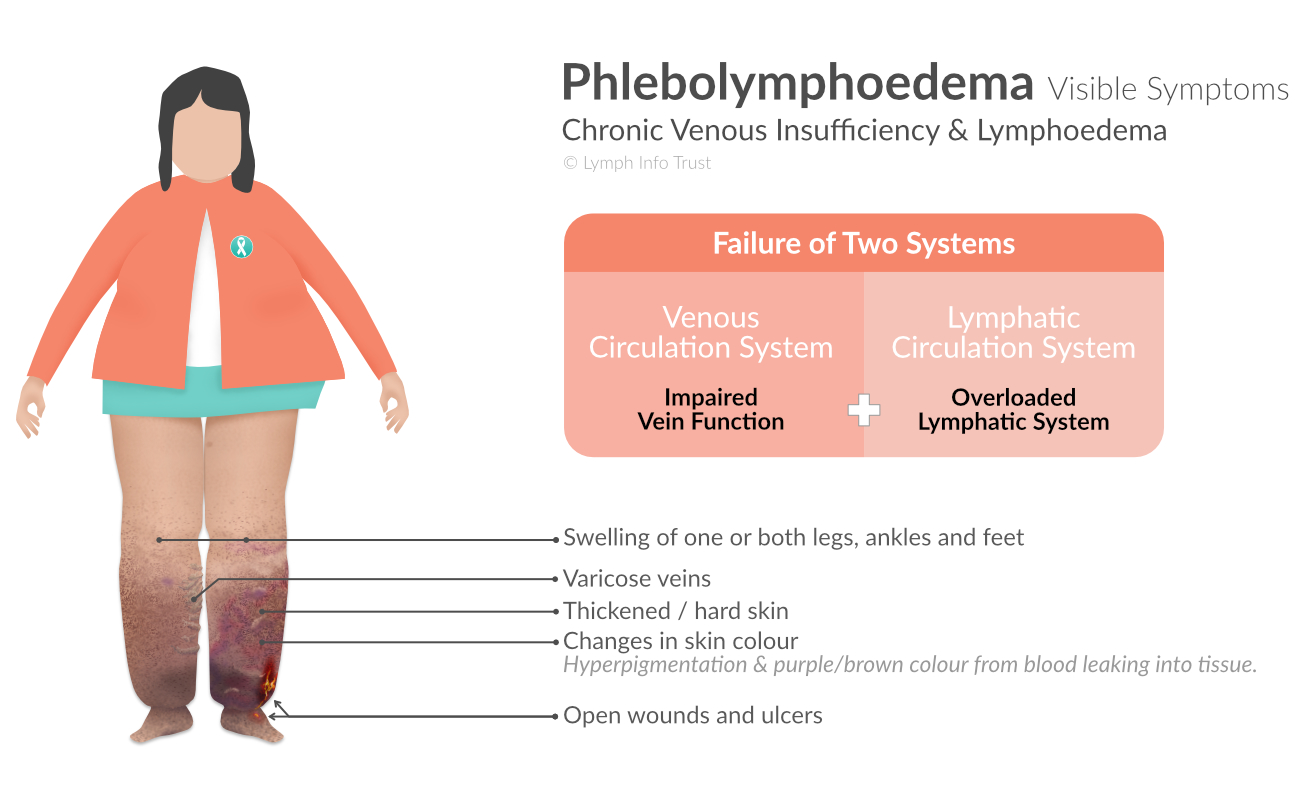
One Leg or Both Legs Affected by Phlebolymphoedema
If you first develop venous insufficiency, both legs are more likely to be affected by phlebolymphoedema.
If you first develop lymphoedema, only one leg may be affected by phlebolymphoedema.
Healthy Veins & Valves
When healthy, the venous and lymphatic circulation systems remove used blood from tissue.
Pushing blood, from your feet and legs, up to the heart takes effort. When standing or sitting upright, there is the pull of gravity to contend with.
Vein valves ensure blood moves in one direction to the heart. The valves prevent blood from flowing in the reverse direction. Contraction of the calf muscle helps push blood to the heart.
Venous Reflux & Venous Insufficiency
When vein valves weaken, they can deform. As a result, the valves do not close when they should. This weakening permits the back-flow (reflux) of blood which can:
- dilate the vein
- weaken the walls of the vein, and
- cause inflammation of the vein.
Venous reflux can develop into several venous diseases, such as:
- varicose veins
These are superficial veins that can become enlarged and twisted. - venous ulcers
These are non-healing wounds that can typically develop around the ankles. - swollen legs, and
Swollen legs may indicate the development of phleboedema which is also called chronic venous insufficiency. - aches or pain.
Ankles that swell during the day and reduce in size overnight indicate the development of venous reflux / venous insufficiency. On its own, venous reflux is treatable by removing the vein's damaged valves, and re-routing blood through healthy veins.
Phleboedema / Chronic Venous Insufficiency
Venous insufficiency can lead to chronic venous insufficiency (CVI), which is also known as Phleboedema.
With the increased strain on the walls of the veins, blood plasma leaks into the spaces between cells of tissue. This in turn causes swelling of the calves, ankles and feet.
Phlebolymphoedema
As phlebodoema becomes more advanced, the lymphatic circulation system compensates for the failed venous circulation system. Phlebolymphoedena occurs when both the venous and lymphatic circulation systems are overloaded.
In addition to the swelling, symptoms can include:
- itching
- pain
- changes in skin colour
Purple or brown staining indicates the leaking of blood into surrounding tissue. - changes in skin texture / hardness
- varicose veins
- fibrosis
Left untreated, lymph fluid turns into a gel, then into a solid mass. It affects toes, feet and ankles. - wounds and chronic ulcers, and
- an increased susceptibility to infection (cellulitis).
Diet and Exercise
Preventative actions include diet and exercise.
Maintaining muscle movement supports blood flow, pushing blood towards the heart.
Underlying Causes
One or more of the following factors can contribute to phlebolymphoedema:
- family history
- pregnancy
- inflamed veins
- varicose veins
- blood clots
- trauma
- damage to legs from surgery .
The following lifestyle factors can lead to venous insufficiency and phlebolymphoedema.
- insufficient exercise
- smoking
- standing or sitting for a long time
- being overweight
Phlebolymphoedema Symptoms
One or more of these visible symptoms can be present in phlebolymphoedema:
- star-shaped scars
These scar remnants will be from an infection or healed ulcer. They are called atrophie blanche. - purple varicose veins
These are dilated veins with a diameter greater than 3 mm. These veins protrude above the surface of the skin and may be painful. - small red spider veins
These are called telangiectasia. - brownish-bronze discolouration
This is known as hyperpigmentation or hemosiderin staining. The discolouration is caused by red blood cells leaking out of the veins; permanently staining the skin. - brown hard patches
These patches are the remnants of a cellulitis infection. - redness at normal leg temperature
This may be a result of widening blood vessels (vasodilation). Elevating the leg can reduce the redness.
Redness can occur in response to heat and inflammation.
Redness is a form of erythema (rash). Treat severe rashes immediately. Severe rashes can be life threatening.
Medications and supportive care will provide comfort, but will not shorten the duration of the redness. - red-purple discolouration
If the ankles are discoloured, itchy, forming sores and thickened skin, this may be stasis dermatitis. Stasis dermatitis can resemble other conditions, for example, cellulitis and contact dermatitis.
If redness is ongoing, seek medical advice.
Risk of Infection
Cellulitis is an infection of the skin. It can be caused by staphylococcus or streptococcal bacteria. The lymph system's ability to destroy bacteria is impaired if you have lymphoedema.
WARNING! A cellulitis infection can be very serious and must be seen immediately by a medical professional.
Signs of cellulitis are:
- redness spreading over an area
- hot skin
- pain
- increased swelling, and
- flu-like symptoms
Fibrosis
Fibrosis is a process where fluid turns into a gel, then into a solid mass. Toes, feet and ankles can be affected.
Fibrosis is more likely to develop when sitting for prolonged periods with feet on the floor.
Elevating the legs when sleeping reduces the likelyhood of developing fibrosis.
By treating the cause (swelling), the progress of fibrosis can be reduced, thereby reducing the progression of lymphoedema.
Diagnosis
A medical professional starts with a thorough medical examination. The examination determines how far the phlebolymphoedema has progressed. The patient's medical history is reviewed to determine any hereditary risks in relation to venous drainage disorder.
An ultrasound can be used to detect where blood may be pooling.
An early diagnosis will better:
- determine how phlebolymphoedema is likely to develop
That is, whether it is likely to get better, remain stable, or worsen. - set expectations on quality of life, and
This includes carrying out everyday tasks, or whether you need support services. - anticipate health issues and complications.
Developmental Stages
Including Stage 0, there are seven recognised stages of phlebolymphoedema. The stages are:
- Stage 0 – No Visible Signs
- Stage 1 – Visible Veins & Blood Vessels
- Stage 2 – Varicose Veins
- Stage 3 – Swelling
- Stage 4 – Skin Changes
- Stage 5 – Ulcers
- Stage 6 – Ongoing
Stage 0 – No Visible Signs
There may be no visible signs (swelling or enlarged veins) of venous insufficiency.
Your doctor may recommend some lifestyle changes if you are overweight.
Stage 1 – Visible Veins & Blood Vessels
At stage 1, veins and blood vessels will be visible but not swollen. These may be:
- reticular veins
These veins are blue or purple, and between 1 and 3 millimetres in diameter. - telangiectasia
These are thin red lines (spider veins), and are less than 1 mm in diameter.
To slow down the development of venous insufficiency, the doctor may recommend:
- lifestyle changes, and
- the use of compression garments.
Stage 2 – Varicose Veins
In stage 2, varicose veins begin to protrude above the skin.
To slow down the development of venous insufficiency, the doctor may recommend:
- exercise
- compression therapy, and / or
- specialist treatment by a vascular surgeon or phlebologist.
In some cases, varicose veins do return.
Stage 3 – Swelling
At Stage 3, the venous circulation system can no longer be compensated for by the lymphatic circulation system. That is, the lymphatic circulation system is now overloaded.
Legs, ankles and feet begin to swell. This indicates the start of Phlebolymphodoema.
Compression therapy is the best method for slowing down the development of phlebolymphoedema.
Stage 4 – Skin Changes
With phlebolymphoedema now established, the skin will change.
These changes progress as follows:
- red and itchy skin
There may also be small brown or grey marks on the skin. - thickened / hard skin
This may be painful scars may develop. - the development of abnormally dilated veins and blood vessels around the ankles
This is corona phlebctatica.
The doctor may recommend skincare products and treatments for managing the swelling, and to treat veinous insufficiency.
Stage 5 – Ulcers
At stage 5, ulcers begin to develop. Open ulcers will heal.
Note: If the ulcers don’t heal, this means you have reached Stage 6 of the condition.
At Stage 5, skincare treatments are still recommended. The doctor may also recommend treatments that help to:
- maximise the efficiency of the venous circulation system, and
- prevent the overload of fluid, thereby reducing swelling.
Stage 6 – Ongoing
To reduce the potential for infection, wounds may need to be treated by a wound care specialist, e.g., nurse. Without treatment, ulcers are likely to return.
First Priority – Wound Care
Ensure wound care is well underway before treating your phlebolymphoedema.
An overloaded venous circulation system will lead to fragile skin and wounds. Combined with a congested lymphatic system, open wounds are susceptible to infection. With all this poor blood and lymph circulation:
- wounds will be slow to heal, and
- ulcers can become an ongoing problem.
With the increased risk of infection, staying on top of wound care is paramount.
Second Priority – Phlebolymphoedema Treatment
See your doctor for a treatment programme. An effective treatment programme will reduce swelling, and slow down or halt the development of phlebolymphoedema.
The treatment programme should include:
- wound care specialists, and
- certified lymphoedema therapists.
A certified lymphoedema therapist can administer Combined Decongestive Treatment. This treatment consists of:
- manual lymphatic drainage
- compressive wraps and garments
- skincare, and
- exercise.
Conservative treatment consists of elevation, exercise, and compression.













